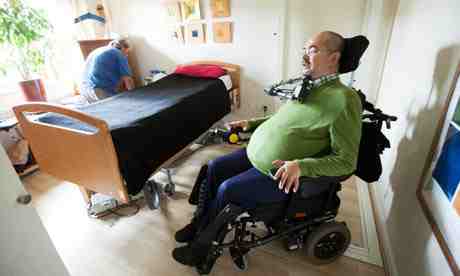
Former Test cricketer Winston Davis’s life was, in his own words, turned upside down when he suffered severe spinal injuries in an accident. Now tetraplegic, the one-time Glamorgan, Northamptonshire and West Indies fast bowler needs round-the-clock help from care staff in his home. It is this care package that allows him to maintain his independence and play an active role with disability rights groups in his community in Bewdley, Worcestershire.
“My 24-hour care allows me to live at home. It makes all the difference – it means you can still participate in your community,” he says. “It’s important to hold on to your normality and self-esteem. It’s lovely to live almost a normal life – to go shopping, to have a social life, to go to church, to visit people, to be involved in activities.”
But now Davis fears many could lose the independence he so values, as Worcestershire county council considers plans to cap the amount it pays for care in the home. Under the plans, which the council admits are controversial, payments for under-65s who need care in their home would be benchmarked, as they already are for older people, with the costs of residential care. Disability campaigners fear the move could force people with physical or learning disabilities into care homes against their will – and set a precedent for other councils as they struggle to reconcile squeezed budgets with increasing demands for social care.
Campaign group We Are Spartacus has warned that the proposals fly in the face of government pledges to help people with disabilities to lead independent lives. “Once this has been done in one council, others will follow and it will become a national problem very quickly,” says Sarah Campbell, co-author of a report on the proposals published by We Are Spartacus.
“This is very worrying for the people of Worcestershire and it’s worrying for people across England. We know councils across the country are trying to save money, and if they see Worcestershire getting away with it, all across England we could see people going back into institutions. We know there is no easy solution to the funding gap, but something that leads to people having to go into homes is not acceptable. We are not living in the 1950s.”
Worcestershire county council admits that the proposals, which are still out for consultation and are due to be considered by councillors in September, may mean people would not get their “first choice” about their care. It stresses that the policy would only apply to new service users and to those whose needs are reassessed. It is a reassurance that has not swayed people with disabilities. Campbell, who is disabled, warns: “The moment your costs are above the cap and you are reassessed, your choice will be either make do or go into a home.”
Worcestershire’s consultation does not put a figure on the residential care costs that will be used to benchmark applications for care packages in the community, but We Are Spartacus says in its report that 2009 rates for a care home placement of £411 a week would mean anyone requiring care six to seven hours a day would be affected. It adds that the alternatives laid out by the council, of individuals topping up payments themselves, reducing the care they receive or applying for help from charities, are just not workable.
In last week’s white paper on social care, the government stressed that it was committed to promoting independence and giving people control over the care they receive. But how can that independence and the consistency of care the paper talks of be achieved in these tough economic times? According to Worcestershire’s head of adult social care, Catherine Driscoll, her authority is “absolutely committed” to the principle of choice. But the council has had to make three-year savings, starting last year, of more than £15.2m on adult social care, with more to come.
“We really need to think about how we can start to have a mature conversation with people about the fact that choice isn’t limitless – there is a financial context,” she says. “We know it’s really controversial, and we haven’t done this lightly at all. We are going through a really full consultation at the end of which cabinet members will consider what’s the most effective way of seeking to put some limits on a needs-led volatile budget.”
The most expensive community care package in the county tops £4,400 a week, with a number costing between £1,500 and £3,000. The maximum expenditure policy could, it is estimated, save £200,000 in its first year. The savings figure was reached by the council looking at the 65 people in 2011/12 who were either completely new to adult social care or whose needs had significantly increased. If the capping policy had been in place, savings could be identified in about half the cases (some had needs that were too complex to be met by an alternative). Driscoll insists the cap would not be rigid, but merely a “comparator for what’s reasonable to meet needs”.
“That is different from saying we are going to force people into residential care,” she stresses. “A young person with a learning disability might want to live on their own with 24/7 support. This policy, if it’s approved, would enable us to say, ‘That’s really expensive and more than we can reasonably justify but would you be interested in working with us to identify other people who might want to live independently in a house with you?’ The costs are then shared.”
Worcestershire is not alone in facing some difficult decisions. Driscoll says other councils are looking at increasing eligibility thresholds for care for disabled people – something Worcestershire says it did not want to do – while others are waiting to see how the capping proposals go.
The Association of Directors of Adult Social Services (Adass) points out that £1.89bn has been taken out of English councils’ adult social care budgets over the last two years. So far, the majority of savings have been achieved through efficiencies and “service redesigns” rather than frontline cuts. But Adass warns that authorities will increasingly have to look for new ways of saving money.
“The longer it goes on, the harder it gets,” says Adass president Sarah Pickup. “Everyone has got to look at ways of managing resources. It’s not surprising that we see people doing what some might call difficult things and some might call thinking outside the box.”
Pickup says that without more resources directed to social care nationally, councils are having to try to “muddle through”. “We have no qualms about the shape of service in the [social care] white paper – it paints a picture of the type of services we would like to be delivering in the 21st century. But in a climate of reducing resources, even with the best possible amount of choice, it’s choice within a framework.”
In Worcestershire, service users agree that a national solution is needed. Like Davis, Simon Heng is tetraplegic and requires round-the-clock care in his home, in his case after a benign tumour damaged his spine. He says his care, which costs around £1,500 a week, allows him to lead an independent life, making his own decisions about his care and contributing to the community, including lecturing on disability issues at a university.
“I appreciate the financial pressures and I don’t think Worcestershire can come up with a solution on its own,” he says. “But this is such a retrograde step. It’s the antithesis of promoting independent living. For people like me, what’s the point of [the taxpayer] spending huge amounts of money to save my life and keep me healthy only to give me a life in confinement? If the council decides it would be cheaper to look after me in care home it would be like giving me a prison sentence.”
guardian.co.uk © Guardian News & Media Limited 2010
Published via the Guardian News Feed plugin for WordPress.
